This story was written by Pip, Mum to 29 Weeker Eloise.
_____________________________________________________________
I had a terrible pregnancy. After the initial excitement of finding out I was pregnant, I have to say that it rapidly turned into the pregnancy from hell. From about 4 weeks the nausea set in and it never left. By 7 weeks I was in hospital and diagnosed with hyperemesis gravidarum – a complication of pregnancy that presents with severe nausea, vomiting, weight loss and dehydration. It is not just morning sickness, it cannot be cured by eating dry crackers or ginger. At best the dehydration caused by constant vomiting can be managed by iv fluids.
I was fortunate enough to have an amazing obstetrician who knew what we were dealing with and was able to admit me to hospital on a regular basis, sometimes one or two times a week to receive iv fluids and medication. We tried everything to help keep the nausea and vomiting at bay - antiemetics, vitamins, acupuncture, ondansetron (a medication most commonly given to patients undergoing chemotherapy), at one stage I was even on steroids which reduced the vomiting from 30 times a day down to about 7 but it came with the price of severe insomnia and rendered me barely able to walk more than 50 metres without feeling like I was having a heart attack. I was weak - physically and emotionally. At first my obstetrician was hopeful that the condition would improve by 14 weeks, it didn’t. He said give it another couple of weeks, still no improvement. By 20 weeks he said that it was likely I would suffer with hyperemesis right up until delivery and that I did.
I remember sitting at my parent’s house that night crying because I simply had no idea how I could possibly make it through another 20 weeks of relentless nausea and vomiting. I’m not going to lie at this point in my story - I lost count of the number of times I wished for the pregnancy to be over. I didn’t know how to make it from one day to the next, sometimes I could only focus on getting through one hour at a time.
I began to fear that when the baby did finally arrive I wouldn’t feel any connection because she was the thing that had made me feel sick for 6 months straight, I feared I would resent her. I often felt that nothing could possibly be worth the torture I was going through (even though to be a mum was all I have ever wanted to be).
Besides the hyperemesis, there were a few other complications to contend with. I have a blood clotting disorder and have a history of deep vein thrombosis so it was decided that the best course of action was that I be placed on blood thinners as a precaution. This meant giving myself clexane injections into my stomach every day from 10 weeks (joy of joys, but my attitude to this was that you do what you gotta do). Next problem – placenta previa. This was detected fairly early on and I was due to get another scan done at about 30 weeks to see how we were tracking with this, but I didn’t manage to make it that far.
On the 20th of December at 29 weeks and 2 days I left home at 10:30am to go to a routine appointment with my obstetrician. I had no idea as I left home that morning that I wouldn’t return for 5 days and that when I did I would be a mother.
I arrived at my obstetrician’s and the nurse took my blood pressure. Once. Twice. It was high but she said it was no cause for concern yet, she would get the doctor to take it again a bit later as women often get a bit anxious when they first arrive at the rooms and it sends their blood pressure up a little.
My doctor came in and he commented that I looked a little puffy around the jaw – in my mind I fobbed this off as probably being a result of the prolonged vomiting. Then he asked if I’d been experiencing any headaches. I get headaches a lot so the answer was yes but I didn’t think much of it. Next question: have you had any visual disturbances like seeing lights? My answer to this was yes - I had been seeing little star like lights but I hadn’t really thought much of it, to be honest I thought it was probably just to do with my almost permanent state of dehydration.
He then took my blood pressure and it was still high and unfortunately at that point I knew where the conversation was heading. My mum had preeclampsia during her pregnancy with my brother so I was familiar with the condition. A quick test of my urine indicated that there was protein and suddenly it was looking more and more like I had developed the same condition. He wrote me a pathology order labelled urgent to go and get another urine test as well as a blood test at Clinpath. So, after our appointment finished off I went feeling slightly annoyed that yet another thing was not right with this pregnancy. He said he would ring me by 5pm that day with the results.
I went and had the blood and urine tests done and I then went over to Mum and Dad’s. It was about 2:30pm in the afternoon and I remember thinking that I felt a bit crampy, like a mild period pain but I really didn’t think anything of it. As I’m writing this I realise it sounds like I didn’t think much about any of these symptoms but please keep in mind that I was in the midst of what I can only describe as having the worst hangover of your life every day for 6 months so I guess I wasn’t really thinking all that clearly. Things changed however when 20 minutes later I felt a gush down below and thought what on earth was that? This definitely wasn’t right. I went to the toilet and saw blood. Still not panicking but knowing something was wrong, I called my obstetrician’s rooms straight away. His staff said to head straight to Burnside Hospital, where I was booked to give birth. About 2 minutes later my obstetrician called and asked how much bleeding I was having and a few other questions and said to go straight to The Women’s and Children’s Hospital and that he would meet me there. Uh oh - this is not good...
I told Mum that we had to go straight to the hospital and as we set off I called my husband to say that there was a bit of a problem and that I was going into hospital. By this stage of my pregnancy I was spending two days a week in hospital for fluids and iv medication and I didn’t really offer him any further details, not wanting to alarm him so he just said okay, and I said I’d call him later.
The journey to the hospital seemed to take forever even though it only took about 15 minutes. By this stage I was starting to get frantic because I could feel that I was losing more blood and by the time we got to the hospital I was so anxious to get inside that I decided that I would make my own way inside before Mum had a chance to find a park. I made it across the road and into the main entrance and then experienced one of the worst moments of my life - I could feel more blood coming out and felt that it was no longer just blood. Doubled over in pain and fear with tears streaming down my face a nurse/ midwife who had finished her shift and was leaving stopped to ask if I needed help. I told her that I needed to get to the Women’s Assessment Service and she put her arms around me and guided me down the long corridors. Had it not been for her help I most certainly would have taken a wrong turn. I will be forever grateful to her for stopping to help me, I had no idea what was happening but I knew that the moment she found me I wasn’t going to lose my baby, not that day anyway. As we walked she tried to gather as much information as she could when we walked through the doors to the WAS. I was put in a wheelchair and taken straight through and hooked up to a CTG machine.
It seemed that my little girl was doing okay, she wasn’t in distress but my blood pressure was through the roof and I was still bleeding and it turned out that what I had felt earlier was the passing of blood clots, suddenly there was talk that my baby might be making her arrival sooner rather than later. It was at this point that I asked my Mum if she could let my husband know what was going on. She called him and told him that he needed to come to the hospital. He still wasn’t aware of the severity of the situation and wasn’t in a particular hurry to leave work so my Mum said to him that this baby could be born tonight! Poor guy nearly fell off his chair and dropped a couple of choice words (not his usual vocabulary in front of my Mum).
The staff at the Women’s and Children’s Hospital were in regular contact with my obstetrician and I was moved up to the High Dependency Unit where he met me. He and another obstetrician did an ultrasound and the look on their faces said it all. They could see a large clot the size of a grapefruit behind my placenta, and he also confirmed that I did indeed have preeclampsia and that sealed my baby’s fate. This baby needed to be born tonight and he said that clot is a ticking time bomb. I would learn weeks later that despite being on blood thinners I had developed several clots which had caused part of my placenta to die, causing the large clot to form behind it. That coupled with the placenta previa and the preeclampsia caused a placental abruption, we were both lucky that we had made it to the Women’s and Children’s to receive the best care available.
As he started to go through what would happen next, he asked if I knew anything about premature babies, if I had ever even seen one. No, I had not. He said that he would try to get a neonatologist to come up and talk to me but I think we ran out of time because the next thing I knew I had the anaesthetist asking me a million questions and I was in theatre before I knew it. And so began the haziest 8 weeks of my life.
I remember 4 things from that theatre.
1. That I absolutely cracked up laughing at something my husband said while I was having the spinal block put in, sometimes if you’re not laughing, you’re crying but it probably wasn’t ideal timing
2. That I had the world’s kindest anaesthetist reassuring me throughout the whole process
3. That I was clinging onto my husband’s hand like I’ve never clung to anything in my life.
4. That my baby girl was born
They brought my little girl around and put her in front of me to look at for about two seconds before the neonatal team descended on her. It would be hours before I saw her again.
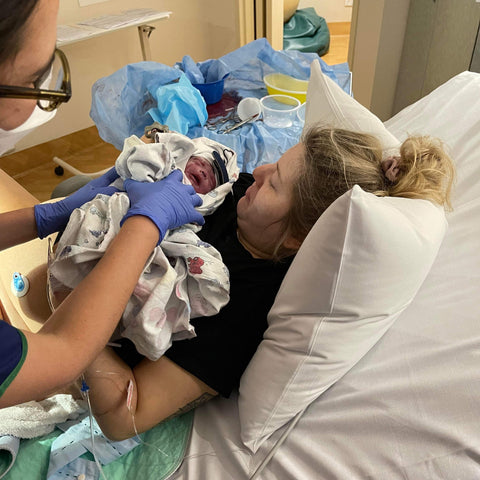
The next time I saw my baby girl was when they wheeled my bed into the NICU. There she was – the tiniest most fragile little thing I had ever seen. All of those fears about not feeling a connection to her were immediately dispelled and I wanted nothing more than to hold her and tell her how much I loved her. But there she was, separated from me in her isolette, covered in wires and tubes and a ventilator. Despite this, I was told that she was in a good condition, this was a good outcome and she was doing surprisingly well.

Meeting in NICU for the very first time

Our first family photo
It wasn’t until late the next afternoon however that I was finally allowed to hold her for the first time. I’m not sure I have the words to describe what a surreal experience this was. I’m sure there is not any mother who doesn’t dream about the moment that she will get to hold her baby for the first time, I don’t think anyone thinks it will be like that though. Attached to CPAP, with wires and lines everywhere, I was so afraid that I would break her. I cried – she was skin and bone. There was no fat on her little body or limbs, she was red, with translucent skin and skeletal, but to me she was beautiful.
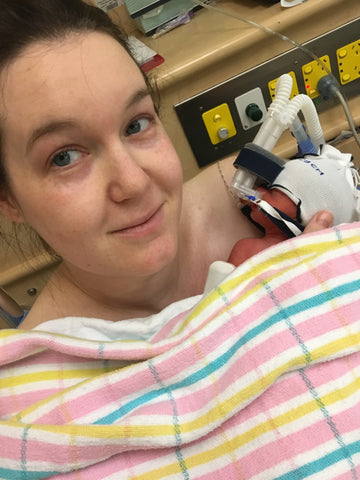
Our First Cuddle
When I saw her the following day she had already graduated to NICU 2, which is when I finally decided that her name was Eloise (we had still been deciding between two names) and a few days later she was moved to SCBU1 – the timeline here is very very hazy. I do remember my obstetrician was amazed though that she was already in SCBU. Her exceptional progress in those first few days was a sign of things to come but that didn’t make the experience any easier for me.
NICU and SCBU life is full of ups and downs. One of the things I struggled with the most was that I felt a huge sense of loss and guilt in those first few hazy weeks. I felt that I wasn’t sure I was even a mother. While I was pregnant, I often felt that I actually wasn’t pregnant, I just felt horrendously sick. I lost weight rather than gaining weight, I couldn’t enjoy any of the usual aspects of pregnancy like getting the nursery ready or a baby shower or watching my belly get big and round. Then I felt like I didn’t really give birth – an emergency caesarean kind of robs you of the birth experience that you had imagined for yourself, especially when you don’t get to hold your baby immediately after. The real icing on the cake though was that even though she had been born, I felt she wasn’t really my baby because there she was, separated from me in her little plastic house. On top of all this I had this soul crushing guilt over all those times I wished for the pregnancy to be over. Yes, I had wanted to get to the finish line, I wanted the sickness to end but never in a million years did I mean for it to end like this. I think that what few people understood and what in the coming weeks some misinterpreted understandably as postnatal depression (thankfully it wasn’t) was that I was grieving this sense of loss and drowning in guilt.
I was discharged from hospital on Christmas Day and it broke my heart that I had to leave her behind. As we left the hospital that morning, a passer-by might have imagined that we were there as visitors because leaving empty handed we certainly didn’t look like overjoyed brand new, first time parents. I lost count of the number of parents I did see leave with their baby and I wondered when it would ever be our turn. I think up until this point I had been coping relatively well but this is where I started to unravel. I hated being apart from her, and I was in a constant state of anxiety that the next time I walked through the doors of SCBU that she wouldn’t be there. I cried myself to sleep every night for about three weeks because I was so afraid that she was going to die. I think that any NICU/SCBU parent can tell you that in this environment nothing ever stays the same. Every day is different, changes in her condition, changes to her feeding, breathing, medication, the amount of time we could spend holding her (which some days was not at all). Nothing was ever constant and I struggled enormously with this, for weeks I felt like I was drowning but I didn’t know which way was up and which was down.
We were so so lucky that for a baby born so early Eloise had a fairly straightforward journey. There were no major complications but she did struggle with apnoea of prematurity and scared me half to death on multiple occasions. I’m not sure anything will ever erase from my memory the first time she had an apnoeic episode whilst I was holding her. Just as I was starting to feel more confident about holding her while she was still attached to Optiflow and various other lines and wires, she stopped breathing – she was bradycardic, having a desat and was turning blue in my arms. Her alarms started blaring and within seconds several nurses swooped on us, scooped her out of my arms and had the situation under control but I was a mess. As I was leaving the hospital that night one of the nurses said to me that the parents of these babies are so brave; they have to be brave to leave and they have to be brave to come back. No truer words were ever spoken – to have to leave her behind each evening required bravery but to walk back in there the next day unsure of what I was about to encounter required bravery too. It is well documented that kangaroo care has a multitude of benefits for the baby and parents and that is what I was doing when Eloise had her apnoeic episode. I was torn between wanting to offer her this care, and of course I longed to spend as much time as possible holding her but after multiple episodes like this it did require a great deal of courage on my part to keep getting her out day after day for a cuddle.
Even though everyone offered encouragement and support, I still felt desperately out of my depth. I was still physically quite unwell from my pregnancy and surgery and was not giving myself time to recover. Nurses, doctors, my husband, my parents all told me that it was okay if I took a day away from the nursery to rest and help myself heal but I couldn’t stay away. For 54 days, I made the journey to and from the hospital, sometimes three times a day (sometimes in the small hours of the morning when I couldn’t sleep for worry).
Despite my worries and fears, Eloise was kicking premmie goals left, right and centre. She was gaining weight, her feeds were increased, we finally got her off Optiflow after numerous attempts, she moved into an open cot and then her monitors were switched off. All these premmie milestones gave me hope that we were moving closer to home. However, the biggest milestone for me and I think the moment that allowed me to really start healing from my grief and sense of loss was the first time I was able to breastfeed Eloise. I was at the hospital late one night having a cuddle when her nurse asked if I wanted to try to breastfeed. She was only 33 weeks at this stage and it was such an unexpected suggestion but I jumped at the chance. With the nurse’s help Eloise latched on straight away and while she only sucked for a minute or two, at that moment in time my heart exploded with love, excitement and pure joy (if only I could bottle that feeling)! I was laughing and crying and kept saying to my husband “look at her! Look at us!” Of course I was excited when Eloise was born and of course I loved her but I think the trauma of her birth and the fact that she was in the NICU meant that I didn’t experience those feelings that most mothers get to experience when they get to hold their baby straight after birth, I still didn’t really feel like she was mine. For me that night was when I got to have that moment and it is a memory I will cherish forever. That moment gave me the strength I needed to keep going for the remaining weeks that Eloise was in SCBU because I finally felt that she was mine. It was the breath of air I needed when I felt like I had been drowning. Slowly we were able to substitute one of her tube feeds for a full breastfeed and there was no looking back – she loved it and I loved it. I eagerly anticipated the next time I could feed her myself. Even now weeks later when I’m at home feeding her I watch her and think back to that night and I can’t help but smile.
Our NICU/SCBU journey finally came to an end 8 weeks after Eloise was born. I don’t know how I can ever thank the doctors, nurses, midwives and other professionals who took care of me and Eloise. I have never seen so many people in one place who are so dedicated to and so passionate about the work that they do. While I have offered my thanks to everyone involved in our care, a special mention does need to go to two nurses in particular – our angels. Not only did they take amazing care of Eloise while she was in SCBU but they took me under their wings and lifted me up on the days that were just too hard. They wiped my tears, they hugged me, the encouraged me and they taught me so much.
And so here we are, all together at home and I can honestly say that I have never been happier. While I’m sure there will be more ups and downs (because as I quickly learnt – the premmie journey doesn’t end after NICU), I feel quite certain that after what it has taken for Eloise and I to get to where we are, we can face any challenge that is thrown our way. She’s my Mini Miracle and I’m her Miracle Mama.


_______________________________________________________________
Thankyou for sharing your story Pip. Eloise is extremely lucky to have such a devoted, brave & loving Mama by her side <3
]]>